Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 920 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

Insert text here
Giovanni Domenico Santorini (1681 – 1737). Italian anatomist, Santorini was born in 1681 in Venice. The son of an apothecary, Santorini studied medicine at Bologna and Padua, receiving his doctorate in Pisa in 1701. He was appointed Public Professor of Anatomy at the Physicomedical College of Medicine when he was 22 years of age.
Santorini was praised for the clarity of his lectures and his dexterity as an anatomist. He used magnifying glasses to study minute anatomical details, allowing him to clearly describe small structures hitherto unknown. Most of Santorini’s biographical data was written by Michael Girardi (1731 – 1797), one of his students. Girardi published Santorini’s work posthumously in 1775 in the book “Anatomici Summi-Septendecim Tabulae”.
Santorini’s himself wrote “Opuscula medica de structura” (Minute Medical Structures) in 1705. His most important book was “Observationes anatomicae”, published in Venice in 1724. One of the most interesting chapters in this book was “De mulierum partis procreationes datis” (Data on the female procreational structures ), making him a pioneer in the teaching of obstetrics. Santorini was physician to the Spedaletto (Hospital) of Venice, where he taught midwifery.
Santorini died in 1737 because of an infection he acquired during the dissection of a cadaver. At that time the rationale for infection and cadaver embalming were unknown.
With his posthumous publications, Santorini’s name and teachings became popular. Today his name is eponymically tied to several structures in the human body:
• Duct of Santorini: An accessory pancreatic duct that opens into a secondary duodenal papilla in the second portion of the duodenum
• Santorini’s valves: Mucosal folds found in the lumen of the primary duodenal papilla (of Vater) or hepatopancretic ampulla
• Santorini’s muscle: Risorius muscle • Santorini’s cartilages: The laryngeal corniculate cartilages
• Santorini’s veins: A plexus of vesicoprostatic veins found in the retropubic space) of Retzius
• Santorini’s concha: The superior nasal turbinate
Sources:
1. “The Dorsal Venous Complex: Dorsal Venous or Dorsal Vasculature Complex? Santorini’s Plexus revisited” Power NE, et al. BJU Inter (2011) 108: 930-932
2. “Giovanni Domenico Santorini: Santorini’s Duct” Edmonson, JM Gastrointest Endosc (2001) 53:6; 25A
3. "Santorini of the duct of Santorini" Haubrich, WS Gastroenterol 120:4, 805
4. “Wirsung and Santorini: The Men Behind the Ducts” Flati, G; Andren-Sandberg, A. Pancreatology (2002)2:4-11
5. "A Historical Perspective: Infection from Cadaveric Dissection from the 18th to the 20th Centuries" Shoja, MM et al. Clin Anat (2013) 26:154-160
- Details
The [conjoint tendon] (sometimes called the conjoined tendon] is the common tendinous attachment of the internal oblique muscle and the transverse abdminis muscle into the pubic tubercle. Some of these tendinous attachments extend also to the pectineal (Cooper's) ligament, the inguinal ligament, and the superior ramus of the pubic bone. In the classical anatomical description these tendons mix to the point that they cannot be separated one from the other, hence the term [conjoint tendon].
The conjoint tendon is important in open hernia repair, where some surgical techniques require the surgeon to pass a surgical needle and suture through this tendinous structure, to attach or close the gap between the conjoint tendon and the inguinal ligament.
In spite of being described in many anatomy books, a true "conjoint tendon" is only found in about 4% of the cases (varying from 3 to 6%, depending on the author). What is usually found are slightly tendinous discrete structures that attach to the pubic tubercle. Because of this, Skandalakis, et al proposed to change the name to the "conjoined area".
Sources:
1. "Le Tendon Conjoint: Memoire realise dans le cadre du certificat d'anatomie, d'imagerie et de morphogenese" Leroux, H. Universite D' Nantes, 2005
2. "Hernia; Surgical Anatomy and Techniques" Skandalakis, J. et al. 1989 McGraw Hill
3. "Tratado de Anatomia Humana" Testut et Latarjet 8 Ed. 1931 Salvat Editores, Spain
- Details
The word "hyaline" is a derivate of the Greek [υαλώδης] (yalódis) meaning "glassy". It refers to a glassy, transparent substance. Although it is usually associated with hyaline cartilage, this term can be used by itself in daily English.
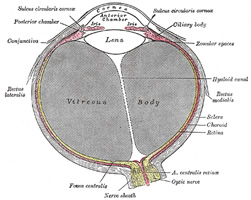
Galen of Pergamon used the term [hyaloid] (glassy, or similar to glass) to refer to the vitreous humor of the eye. As a result of this early anatomical term, today we have the following:
• Hyaloid membrane: also known as the vitreous membrane. It is a collagenous membrane separating the vitreous humor from the rest of the structures of the eye
• Hyaloid artery: a branch of the opthalmic artery which dissapears before birth
• Hyaloid canal: a small membranous canal in the vitrous humor extending between the lens and the optic disc. This can be seen in the accompanying image of a horizontal section of the eye.
Sources:
1. “Gray’s Anatomy” Henry Gray, 1918
2. "Tratado de Anatomia Humana" Testut et Latarjet 8th Ed. 1931 Salvat Editores, Spain
3. "Gray's Anatomy" 38th British Ed. Churchill Livingstone 1995
4. "The Origin of Medical Terms" Skinner, HA 1970 Hafner Publishing Co.
Image modified from the original by Henry VanDyke Carter, MD. in the book "Grays's Anatomy" by Henry Gray FRS. Public domain
Note: Google Translate includes the symbol (?). Clicking on it will allow you to hear the pronunciation of the word.
- Details
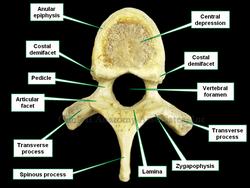
[Anular] means "ring" or "ring-shaped". The word [epiphysis] is composed of the preffix [epi-] meaning "outer" or "above", while [-physis] means "growth". The term [anular epiphysis] means the "outer ring-shaped growth".
The [anular epiphysis], sometimes also called the [anular apophysis], is a bony ring found on the superior and inferior aspect of the vertebrae. This outer ring is formed by thickened cortical bone and leaves a central depression which has a more porous surface. In this central depression the vertebrae present with a thin layer of hyaline cartilage, which forms part of the vertebral endplate.
In a lateral view the presence of the anular epiphysis causes the superior and inferior borders of the vertebral body to protrude. This protrusion is called by some anatomists the "lips" of the vertebrae. To see these "lips" click here.
Image property of: CAA.Inc.Photographer: David M. Klein
- Details
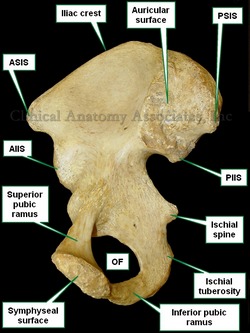
The root term [-auricul-] arises from the Latin word [Auricula], which is a diminutive of [auris] meaning "ear". Auricula means "a little ear".
The adjectival form [auricular] is used in several places in human anatomy. One of them is the [auricular surface of the iliac bone] (see image) referring to a roughened area in the medial aspect of the iliac bone where it articulates with the sacrum, forming the sacroiliac joint. The Latin term for this articular surface is facies auricularis ossis ilii. A corresponding auricular surface is found in the sacral bone, the facies auricularis ossis sacri.
[Auricular] is also used in the term [auricular cartilage], referring to the fibrocartilage found in the ear or [pinna].
A shortened version is the root term [-aur(i)-], meaning the same. It is used in the word [auricle] referring to the atrial appendages of the heart. These appendages when seen from the outside of the heart really look like little "boxer's ears". This image (click here) shows the left atrial appendage (LAA) or left auricle.
By the way, did you know that one of the digits was called "digitus auricularis"? Read the story here.
Image property of: CAA.Inc.Photographer: David M. Klein
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.
Enrique Finochietto, MD (1881 – 1948) Argentinian surgeon and researcher, Enrique Finochietto was born in 1881 in the city of Buenos Aires. He studied in both public and private schools, entering medical school at age 16. He received his medical degree from the University of Buenos Aires in 1904.
Shortly after graduation, he became an intern at the Rawson hospital of Buenos Aires. Dr. Finochietto would become part of the staff of this hospital and be part of its staff all his life. He traveled to Europe to study with surgeons such as Calot, Kocher, Roux, and others, visiting France, Switzerland, Austria, and Italy.
Upon his return he dedicated himself to surgery and endoscopy, and with the help of his brother Ricardo started research and invented many medical and surgical devices, including a motorized surgical table, endoscopic devices and surgical instruments, some of which are in use today throughout the world.
During World War I Dr. Finochietto worked for no fee (ad honorem) as surgeon-in-chief at the Argentine Hospital in Paris. For his dedication and work, France awarded him the Legion d’Honneur and the Red Cross. He came back to Argentina and then traveled to the USA where he visited with the Mayo Brothers and Harvey Cushing. One of Dr. Finochietto’s mottos was “Only the surgeon who goes beyond his obligations serves his duty”.
Although mostly remembered for the Finochietto rib spreader, Dr. Finochietto tackled most types of surgery during his career, including neurosurgery, gastrointestinal, thyroid, thoracic, and orthopedic.
Dr. Finochietto died on February 17, 1948. His legacy in Argentinian surgery lives on through his school of thought, research and disciples.
If you click on Dr. Finochietto’s image (courtesy of Wikipedia) you will see an image of his namesake rib spreader (courtesy of Surgiway, France ).
Sources:
1. “Memoir: Enrique Finochietto, MD (1881 – 1948)” DeBakey. ME. Ann Surg. 1948 Aug; 128(2): 319–320
2. “Enrique Finochietto” The Legacy of Surgery in Argentina” De La Fuente, SG. J Surg Ed (2007)64:2; 120-123
3. “El separador intercostal de Enrique Finochietto, el hospital Rawson, la escuela quir?rgica, y una an?cdota que los relaciona” Saadia, A. Rev Arg Cir Cardiovasc (2009) 3:3 149-150
4. “Rese?as hist?ricas: Enrique Finochietto” Parquet RA. Acta Gastroenterol Latinoam (2009); 39:18
5. “Surgery in Argentina” Beveraggi, EM. Arch Surg (1999) 134”438-444
6. “The Legends Behind Cardiothoracic Surgical Instruments” Ailawadi, G et al. Ann Thorac Surg (2010) 89:5; 1693-1700