Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 259 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
- Written by: Prof. C. Uribe
|
Anatomy:[Hilum] is a generic term which names area of an organ where all the structures that enter or leave the organ are found. In the lung it is depression in the mediastinal surface of the lung through which the vessels and bronchi enter and leave the lungs. This set of structures corresponds to the “root of the lung” or “pulmonary pedicle”. The term has a singular form, [hilum]; and a plural form, [hila]; the adjectival form is [hilar]. Radiographs and CAT Scan: The hilum appears as a composite opacity at the root of each lung produced by bronchi, arteries, veins, lymph nodes, nerves ,and other tissues. Sources: |
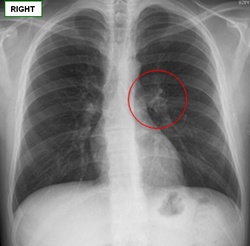 AP thoracic x-ray image showing the pulmonary hilum |
| Back to MTD Main Page | Subscribe to MTD |
- Details
We would like to welcome Professor Cristián Uribe as a contributor to Medical Terminology Daily.
Prof. Uribe is a Physical Therapist, has a Masters in Human Anatomy and is a Professor in the Human Anatomy Department of the Medical School at the University Finis Terrae in Santiago, Chile.
Prof. Uribe is also the Director of the Postgraduate Course on “Anatomical Bases of Normal Imaging”, as well as the Executive Secretary of the Postgraduate Office at the same University.
He published the book “Eponyms in Anatomical Nomenclature” (2011, Ed. U. Finis Terrae). For his LinkedIn page click here.
- Details
The [valve of the inferior vena cava] is probably better known by its eponym, the [Eustachian valve]. This is an incomplete valve found at the most distal end of the inferior vena cava, at the point where it opens into the right atrium of the heart. The valve is muscular at its base and composed mostly by membranous endocardium, and is normally the only valve present in the inferior vena cava.
It appears as a membranous semilunar fold extending posteriorly from the limbus fossa ovalis, anterior to the inferior caval orifice where it disappears. Its free border is usually membranous, concave, and directed anterosuperiorly. Its base is a transverse muscular ridge continuous with the anterior margin of the caval orifice.
It has no function in the adult, but in the fetus it helps to divert the flow of blood coming from the inferior vena cava towards the foramen ovale [fossa ovalis], as part of fetal circulation.
It has great anatomical variation in size, shape and thickness. On its medial aspect it joins with the Thebesian valve at the orifice of the coronary sinus.
First described by Bartolomeo Eustachius (c1500 - 1574) in 1653, the existence of the valve of the inferior vena cava was disputed by many until Winslow in 1717 confirmed its presence and suggested its function in fetal circulation.
Sources:
1. "The Valve of the Inferior Vena Cava" Hickie, JB Br Heart J. 1956 Jul; 18(3): 320–326
2. "Bartolommeo Eustachio; a great medical genius whose masterpiece remained hidden for 150 years" Wells, WA Arch Otolaring (1925) 48: 58
- Details
The medical word [dysphagia] arises from the suffix [dys-] which means "abnormal", the root term [phag-] which arises from the Greek [φάγος] (phagos), meaning "to swallow", a "glutton" or "eating much", and the suffix [-ia] meaning "condition". The word dysphagia then means "a condition of abnormal swallowing".
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

Bartolomeo Eustachius
Bartolomeo Eustachius (c1500 - 1574) Italian physician and anatomist, also known as Bartholomew Eustachius, Esutachi, and e was born in the small town of San Severino Marche, in the province of Macerata, central Italy. His father was a respected physician, and may have attended as a student the University of Sapienza, where he later taught as a professor of practical medicine. Eustachius’ life is mostly unknown and some of his works remained hidden for over 150 years. His birth date is only an estimate and data varies from c1500 AD to c1510 AD.
It is known that Eustachius lived and worked in Rome from 1549 to 1574. He was both an anatomist and a physician to the Vatican. As an anatomist, Eustachius is credited for having been the first to prepare anatomical images for printing using copper plates.
As a hospital physician, Eustachius was adamant on the need of autopsies on patients who died at the hospital, crediting him with being one of the first pathological anatomists.
Eustachius’ is credited with several anatomical discoveries, which he published in short monographs, on topics like the kidneys, the suprarenal glands (which he was the first to describe), the movements of the head, the azygos vein, etc. One of these was entirely dedicated to dentistry, “Libellus de Dentibus”, which have led to some to call Eustachius “The Father of Dental Anatomy”.
Eustachius dedicated himself to prepare a number of anatomical copper plates, apparently getting ready to publish a book to rival Vesalius’ “Fabrica”. It is known that Eustachius disliked Vesalius because of Vesalius’ contempt for the teachings of Galen. Eustachius died before completing his work and the copper plates were forgotten for over a century. After being rediscovered, these plates were published with commentaries by anatomists, until a final publication in Latin by Bernard Siegfried Albinus (1697 – 1770) entitled “Explicatio Tabularum Anatomicarum Bartholomaei Eustachii Anatomici Summi” (An explanation of the Anatomical Picture of Bartholomew Eustachius, Supreme Anatomist”.
Besides the suprarenal gland, Eustachius is credited for having discovered the stapes, the tensor tympani muscle, the valve of the inferior vena cava, the cervical sympathetic chain and the thoracic duct.
Interesting note: Eustachius’ assistant Petrus Matthaeus Pinus, who helped develop the copper plates, voiced his master’s dislike of Vesalius in a poem that was published by Albinus over a hundred years after the death of all of them, it is also an epitaph for a great anatomist:
“Just as the Master from Pergamon (Galen)
Teaching his method of healing, once refuted
The false writings of the ignorant Thessalus,
So also my BARTOLO (Eustachius)
Teaching his method of denoting every detail, position,
Shape, structure, order, number and condition
Has repulsed the shameless arrogance and claims
Of the impudent Vesalius
To him (Eustachius) all future generations
Adhere In reverential admiration
The age to come will envy us on account of you Father,
And historians will wish they had lived sooner
They will extol our era, through you fortunate,
Lucky beyond measure"
Sources:
1. "The root of dental anatomy: a case for naming Eustachius the "Father of Dental Anatomy"" Bennett, G (2009) J Hist Dent (1089-6287), 57 (2) 85 -88
2. “The papal anatomist: Eustachius in renaissance Rome” Simpson, D, ANZ J Surg (2011) 81: (12)905 -910
3. “Bartholomeo Eustachio – The Third Man: Eustachius Published by Albinus” Fahrer, M. (2003) ANS J Surg; 73: 523- 528
4. "Bartolommeo Eustachio; a great medical genius whose masterpiece remained hidden for 150 years" Wells, WA Arch Otolaring (1925) 48: 58
Original image courtesy of: Wikimedia Commons.
- Details
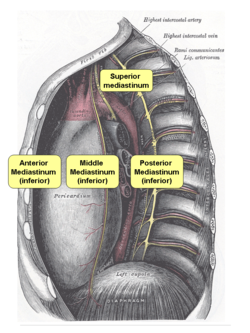
UPDATED: The mediastinum is the median region of the thorax, usually described as the "space"1 between the lungs. This region is divided into a superior and inferior mediastinum by a plane that pases through the sternal angle or Angle of Louis.
The inferior mediastinum is itself divided into three separate regions by the pericardial sac. The region anterior to the pericardial sac is the "anterior mediastinum", the region posterior to the pericardial sac is the "posterior mediastinum", and the region containing and including the pericardial sac is the "middle mediastinum". Thus described the mediastinum comprises four regions as follows:
• Superior mediastinum: It contains the aortic arch, the brachiocephalic trunk, the thoracic segments of the left common carotid and the left subclavian arteries, the brachiocephalic veins, a portion of the superior vena cava, the vagus nerve, phrenic nerve, and left recurrent laryngeal nerve, trachea, esophagus, thoracic duct and the remains of the thymus gland
• Anterior mediastinum: A narrow space, more developed on the left side, anterior to the pericardial sac and contains some lymph nodes and connective tissue
• Middle mediastinum: The largest mediastinal region, it contains the pericardial sac, the heart, the bifurcation of the trachea, the inferior vena cava, and the cardiac end of the great vessels.
• Posterior mediastinum: Contains the descending aorta, the azygos and hemiazygos veins, the esophagus, and thoracic duct.
Personally, I do not use the description of the mediastinum as a "the space beween the lungs", as it conjures the image of literal "open spaces" around or between the organs. The fact is that the mediastinum is tightly packed with no spaces between the organs. This is why I prefer the definition of the mediastinum as an "area" or "region" between the lungs. Dr. Miranda.