Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 2437 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
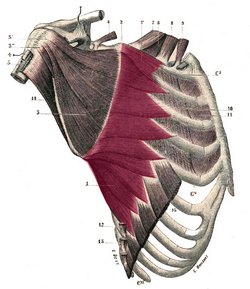
The serratus anterior or serratus magnus is a is a wide, thin muscle sheet situated on the posterolateral aspect of the thorax and extends between the ribs and the scapula. It is formed by well-defined separate muscular digitations that originate in the external surface and superior aspect of the first superior eight (or nine) ribs. These originating fibers also arise from the fasciae covering the intercostal muscles. This is especially true for the first or most superior digitation which arises from the first and second rib and the intervening external intercostal fascia.
These digitations cover the lateral aspect of the thorax, pass deep to the scapula and converge to insert on the deep aspect of the medial border of the scapula. Some of its fibers may even hug the medial border of the scapula and insert on its anterior aspect. The first digitation is inserted into a triangular area on the ventral surface of the medial scapular angle. The next two digitations spread out to form a triangular sheet, the base of which is directed posteriorly and is inserted into nearly the whole length of the ventral surface of the vertebral border. The lower five or six digitations converge to form a fan-shaped mass, the apex of which inserts into a triangular impression on the ventral surface of the inferior scapular angle. The lower four slips of the serratus anterior interdigitate with the superior five muscular slips of the external oblique muscle.
This muscle receives its nerve supply from the long thoracic nerve, (ventral rami of C5-C7), arising from the roots of C5, C6, and C7 (sometimes absent) of the brachial plexus
The word “serratus” derivates from the Latin word [serro] meaning “saw”. Serratus means “serrated” referring to the multiple tooth-like anterior digitations of the muscle. The plural form for "serratus" is " serrati". The Latin term “magnus” means “great”, “large”, or “mighty”. It points to the fact that this is the largest of three muscles that carry the same name “serratus”. The other two are the serratus posterior superior and the serratus posterior inferior.
The serratus anterior is one of the 17 muscles that attach to the scapula.
Note: The image shown in this article is from “Gray’s Anatomy” by Henry Gray (1918) which is in the public domain. It depicts the serratus anterior in situ and shows the scapula retracted posteriorly. The scapula is covered on its internal aspect by the subscapularis muscle (number 3 in the image). A better image can be found in “An Illustrated Atlas of the Skeletal Muscles” by Bowden (2015) which we cannot publish for copyright reasons.
Sources:
1. “Gray’s Anatomy” Henry Gray, 1918
2. "Tratado de Anatomia Humana" Testut et Latarjet 8th Ed. 1931 Salvat Editores, Spain
3. "Gray's Anatomy" 38th British Ed. Churchill Livingstone 1995
4. “An Illustrated Atlas of the Skeletal Muscles” Bowden, B. 4th Ed. Morton Publishing. 2015
Image modified from the original by Henry VanDyke Carter, MD. Public domain
- Details
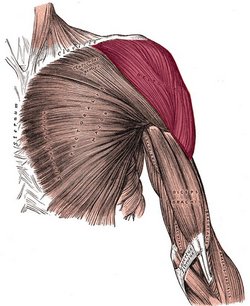
The deltoid or deltoideus (Latin) is a large, thick, triangular muscle, which covers the glenohumeral joint anteriorly, superiorly, and posteriorly. It can be described as having three components or segments, anterior, middle, and posterior. The anterior portion originates from the lateral third of the clavicle, on the clavicle’s superior border. The middle portion originates from the lateral border of the scapula’s acromion, and the posterior portion originates from the spine of the scapula. All three portions insert laterally by means of a thick tendon on the deltoid tuberosity of the humerus. At its insertion the muscle gives off an thick connective tissue expansion to the deep fascia of the arm.
The three portions of the deltoid muscle are usually well defined. As an anatomical variation, the clavicular or the acromial portion of the muscle may be absent.
This muscle is innervated by the axillary nerve (C5, C6), a branch of the brachial plexus, and supplied by the posterior circumflex humeral artery and the deltoid branch of the thoracoacromial artery.
The word deltoid is derivates from the Greek word [δελτοειδής] which is itself formed by the terms [δέλτα] (délta), referring to the triangular shape of the letter delta (uppercase Δ, lowercase δ) and [-οειδής] (-oeidís), a the Greek suffix meaning “similar to”. Delt-oid then would mean “similar to a Δ (delta)".
The deltoid is one of the 17 muscles that attach to the scapula.
Sources:
1. “Gray’s Anatomy” Henry Gray, 1918
2. "Tratado de Anatomia Humana" Testut et Latarjet 8th Ed. 1931 Salvat Editores, Spain
3. "Gray's Anatomy" 38th British Ed. Churchill Livingstone 1995
4. “An Illustrated Atlas of the Skeletal Muscles” Bowden, B. 4th Ed. Morton Publishing. 2015
Image modified from the original by Henry VanDyke Carter, MD. Public domain
- Details

We are proud to announce that our own contributor and associate Dr. Elizabeth Murray, Ph.D., has been awarded the Anthropology Section's 2018 "T. Dale Stewart Award" at the American Academy of Forensic Sciences (AAFS) 71st Annual Scientific Meeting in late February.
Dr. Murray's involvement with AAFS has included chairing the Academy-wide annual meeting as well as committee-level service in long-term planning, Board of Trustees, and the Student Academy.
Well-known and respected as a forensic anthropologist, Dr. Murray teaches at the University of Mount St. Joseph courses in anatomy and physiology, gross anatomy, and forensic science for the Department of Biology. Her most recent book, published in 2019, is "The Dozier School for Boys: Forensics, Survivors, and a Painful Past."
Our congratulations to her for yet another incredible achievement in her illustrious career. We are glad to count her as a friend and as a contributor to "Medical Terminology Daily" and Clinical Anatomy Associates, Inc.
- Details
- Written by: Prof. Claudio R. Molina, MSc
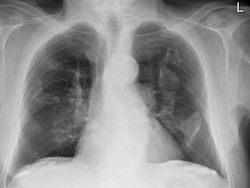
Holly leaf sign.
Click on the image for a larger depiction
The Holly is a tree/shrub of the genus Ilex , with perhaps the most well know being Ilex aquifolium. The plant has shiny prickly evergreen leaves and bright red berries. Cut branches of Holly are widely used as a traditionally Christmas decoration especially in wreaths and Christmas cards as illustrations. “The Holly and the Ivy” is a popular traditional English Christmas carol.
The [Holly leaf sign] refers to the appearance of calcified pleural plaques seen on chest radiographs. Pleural plaques are common in patients who have been exposed to asbestos, are asymptomatic and are most useful as a marker of asbestos exposure or asbestosis. They can be identified in 3-14% of dockyard workers and in 58% in insulation workers.
They are themselves not malignant, but patients with this plaques have a greater risk of mesothelioma and bronchogenic cancer than the general population and patients with exposed to asbestos but not pleural plaques.
The plaques arise in the parietal pleura and have predilection for the diaphragmatic dome and the undersurface of the lower posterolateral ribs. Rarely involve the visceral pleura but occasionally they are found in the fissures of the lungs.
On plain radiographic plaques appear as a geographic, usually calcified, opacities with irregular but well-defined edges. The irregular thickened nodular edges of the pleural plaques are likened to appearance of a Holly leaf, which has sharp spines along its margin.
Sources:
1. Jane R, Gulati A., Dwivedi R., Avula S., Curtis J., Abernethy L. (2013) We wish you a Merry X-Ray-mas: Christmas signs in radiology. BMJ 347:f7020 doi: 10.1136/bmj.f7020
2. Walker C., Takasugi J., Chung J., Reddy, G., Done S., Pipavath S., Schmidt R., Godwin J. (2012). Tumor-like Conditions of the Pleura. Radiographics 32:971–985.
3. Case radiograph courtesy of Dr Çağlayan Çakır, Radiopaedia.org. From the case rID: 22986
Figure below. Ilex aquifolium. Courtesy of A.Prof Frank Gaillard, Radiopaedia.org. From the case rID: 12398

Holly leaf sign.
Click on the image for a larger depiction
Article submitted by: Prof. Claudio R. Molina, MsC.
- Details
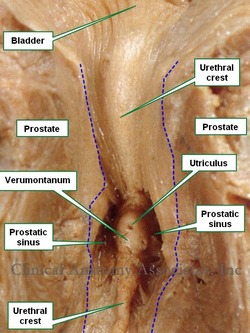
Anterior view of a section of the prostate gland. The blue
dotted line shows the edges of the prostatic urethra
[UPDATED] The [prostatic utricle], also known as "utriculus prostaticus" or "utriculus" is a small 6 mm small dead-end channel found in the male prostatic urethra.
The word [utriculus] is Latin and means "little sac"..
What is interesting about this structure is that it is the embryological remnant in the male of the Müllerian ducts that form the vagina and the uterus in the female. In fact, in some texts the prostatic utricle is referred to as "uterus masculinus". Some researchers differ and point to the fact that this structure may not be a Müllerian duct derivate.
The prostatic utricle is found inside the prostate, forming part of the posterior wall of the prostatic urethra. It is in the upper part of a small mound which is part of the prostatic crest. This mound is called the [colliculus seminalis] or [verumontanum], which is Latin and translates as the "mountain or mound of truth". On the verumontanum are the two slit-like openings of the ejaculatory ducts. Lateral to the verumontanum are the prostatic sinuses, depressions where the prostatic ducts are found.
Sources:
1. "The prostatic utricle is not a M?llerian duct remnant: immunohistochemical evidence for a distinct urogenital sinus origin" Shapiro E, Huang H, McFadden DE, et al. (2004) J Urol 172; 1753–1756
2. "Gray's Anatomy"38th British Ed. Churchill Livingstone 1995
3. "Tratado de Anatomia Humana" Testut et Latarjet 8 Ed. 1931 Salvat Editores, Spain
- Details
- Written by: Efrain A. Miranda, Ph.D.
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

Jane Todd Crawford - Daguerrotype
When writing the article “The Ephraim McDowell House and Museum” I realized that there are so many patients that by volunteering to a novel or sometimes experimental procedure or donating their bodies have been the catalyst of the advancement of medical science, surgery, and anatomy. Benigno says it so clearly in his paper explaining the physician/patient relation of McDowell and his patient: “Because of his innovative genius and finally honed surgical skills, Ephraim McDowell gave Jane Todd Crawford her life, and she, in return, gave him immortality”.
Few patients have influenced local history more than Jane Todd Crawford. In Kentucky there is a road named after her, a hospital bears her name in Greenville, KY, and there is even a formal "Jane Todd Crawford Day" on December 13!
By contrast, there are so many unknown patients whose names history has forgotten, and yet the fame of the physician continues through time in eponymic hospitals, educational institutions, named surgical procedures or maneuvers, surgical instruments, etc.
Some of the names and stories have survived, but many have not. In some cases, we know the name, but little else.
Dr. Henry Heimlich used his “Heimlich maneuver” for the first time to save his neighbor Patty Ris, in 2016, forty-two years after publishing it in 1974. The maneuver itself was used that same year (1974) to save the first person, Irene Bogachus, who was choking at a restaurant. Hundreds of thousands of people have been saved from death from choking by the proper use of this maneuver.
Dr. Christiaan Barnard, performed the first successful heart transplant on December 3, 1967. We know the name of the donor, 25 year-old Denise Darvall, and the recipient Lewis Washkansky.
Dr. Antoine Dubois and Dr. Dominique-Jean Larrey in France performed the first mastectomy on September 30, 1811. This was decades before the advent of anesthesia or aseptic technique. The patients was Fanny Burney, a famous novelist.
Dr. Edward Jenner developed the smallpox vaccine after working with a milkmaid, Sarah Nelmes. Jenner’s work saved the Americas from the smallpox epidemic through the work of Don Antonio de Gimbernat y Arbós and Don Francisco Javier de Balmis i Berenguer and his “Balmis Expedition”
The examples can continue, but who was the patient on the first Billroth procedure, who was the patient in the first Scopinaro procedure? Who was the patient on whom Dr. Eric Muhe performed the first laparoscopic cholecystectomy? Many are unknown yet they helped pave the way of the future.
The same can be said for the world of human anatomy. Today we honor the donors who will their bodies so that future physicians can study the intricacy of the human body, but we never know their names or their stories. Many a time I have stood at the side of a body while medical students dissect and study and wondered about their identities, the life they had, and what led them to give us their bodies as a wonderful gift to science and medicine.
There was a time (long ago) when the dissection of a human body was punished by the Church, or the times when the scarcity of bodies was such that some started to rob graves, or when the punishment for a crime was “death and a public anatomy”.
Some of these people we know, most of them we do not. Some have given their body willingly, others have not.
Joseph Paul Jernigan, a murderer, who after given the death penalty, donated his body to a now world-renown endeavor, the Visible Human Project.
The oldest known anatomical preparation is a skeleton mounted in Basel (Belgium) by Andreas Vesalius in 1543. The skeleton belongs to Jacob Karrer von Geweiler, a bigamist and attempted murderer who was beheaded for his crimes.
It is sad that we know the names of these criminals, and in some cases not that of their victims.
We do not know the names of many who, during the Nazi regime in WWII, were taken from concentration camps for medical experiments and as we understand, possibly murdered and dissected to illustrate now infamous anatomical atlases. Research is being done to discover their identities.
Times have changed and body donation has become accepted and praised by society. I am always touched by the words of Morgagni above the entrance to the dissection rooms at the University of Cincinnati: “hic locus est ubi mors gaudet succurrere vitae” meaning “in this place death rejoices helping the living”. The University of Cincinnati has an Annual Memorial Ceremony to honor the body donors and their families. A video of the ceremony can be watched here.
I cannot but end this article with the words that are found in the left side column of this blog and will always be there:
“Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.