Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 357 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
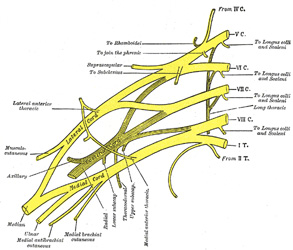
UPDATED: The term [plexus] comes from the Latin term [plectere] meaning " to twine, or to braid". In anatomy, the term [plexus] refers to a group of structures that are intertwined or form a meshwork. The plural form is [plexuses], although the Latin plural form [plexi] is also correct. Gabrielle Fallopius used the term to denote "a tangle of nerves"
There are many plexuses described in the human body. Most are formed by nerves, but there are many that are lymphatic or vascular. The best known are the plexuses of nerves formed by the ventral rami of the spinal nerves. These are the cervical plexus, the brachial plexus, the lumbar plexus, and the sacral plexus. The image depicts the brachial plexus. For a larger version, click on the image, and for further information on the cervical and brachial plexuses, click here.
Images and links courtesy of:www.bartleby.com
- Details
- Written by: Efrain A. Miranda, Ph.D.
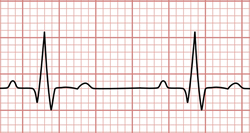
Sinus rhythm electrocardiogram
A contraction, from the Greek [διαστολη] (systolí) meaning “expansion, dilation, drawing out, or prolongation”, also [διαστέλλειν] (diastéllein) meaning “to open, expansion”. When used in music, it means "a pause".
It refers to the dilation of the heart. If you analyze a normal heartbeat (sinus rhythm), there are two diastoles: an atrial diastole and a ventricular diastole. The term diastoleis usually used in reference to the ventricular diastole.
Diastole was first recognized and named by Herophilus of Alexandria (325-255BC), most probably trough animal vivisection. Herophilus was accused of animal vivisection and the dissection of human cadavers. Because of this, some call Herophilus "The Father of Anatomy".
Galen of Pergamon (129AD - 200AD) used the term [διαστέλλεσθαι] (diastéllesthai), also meaning “expansion”.
The word in English was first used in the 16th century. The modern pronunciation in English follows the Greek pronunciation by ending the word in a long “e” as in “to be”.
Sources
1. "The Origin of Medical Terms" Skinner, HA 1970 Hafner Publishing Co.
2. "Medical Meanings - A Glossary of Word Origins" Haubrich, WD. ACP Philadelphia
3. "Dorlands's Illustrated Medical Dictionary" 26th Ed. W.B. Saunders 1994
4. "Greek anatomist Herophilus: the father of anatomy" Si-Yang, N. Anat Cell Biol. 2010; 43(4): 280–283
Note: Google Translate includes an icon that will allow you to hear the pronunciation of the word
- Details
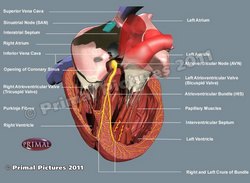
Conduction system of the heart
[UPDATED] The conduction system of the heart is part of a complex intrinsic heartbeat and rhythm control system that includes a cardiomyocyte-based component which acts as an automatic base, and an extrinsic and intrinsic autonomic nervous system component which acts as a modulator.
The classic description of the conduction system of the heart emphasizes only the cardiomyocyte-based component and refers to a group of specialized cardiac muscle structures that serve as pacemakers and distributors of the electrical stimuli that make the heart beat coordinately. It is important to stress the fact that this primary "conduction system of the heart" is not formed by nerves but rather by specialized cardiac muscle cells.
Components of the cardiomyocyte-based conduction system of the heart:
• SA node: The sinoatrial (SA) node is a small nodule of cardiac muscle tissue, somewhat horseshoe-shaped that is found at the junction of the superior vena cava and the right atrium. It receives blood supply from the SA node artery, a branch of the right coronary artery. Later research indicates that the pacemaker function of the SA node includes areas of the lateral wall of the right atrium which are involved in different heart rate speeds. It is also known eponymically as the "node of Keith and Flack" after Sir Arthur Keith (1866 - 1955) and Martin Flack, CBE (1882 - 1931).
The electrical impulses propagate between the right and left atria by way of the interatrial bundle, also known as "Bachmann's bundle", and between the SA node and the atrioventricular node by way of three internodal tracts, described by Karel Frederik Wenckebach (1864–1940), and Christen Thorel (1880 - 1935). More information on these internodal tracts here.
• AV node: The atrioventricular (AV) node is found at the junction of atria and ventricles in an area known as the "Triangle of Koch". Its function is to delay the electrical impulse passing from the atria to the ventricles by 1/10th of a second, enabling the sequential pumping action of the heart. The eponymic name for the AV node is "node of Aschoff-Tawara", and it receives its blood supply by way of the AV node artery, a branch that usually arises from the right coronary artery
• AV bundle: Also known as the "Bundle of His", this thick bundle of specialized myocardial cells is found in the interventricular septum. It divides into the right and left bundle branches
• Bundle branches: Sometimes known as the "crura" of the bundle of His, these two divisions of the AV bundle help distribute the electrical stimuli to the ventricular walls. The right bundle branch has an extension that crosses the lumen of the right ventricle, from the base of the anterior papillary muscle to the interventricular septum, forming a cord of tissue known as the "moderator band" or "septomarginal trabecula"
• Purkinje Fibers: These thin fibers are the terminal end of the conduction system of the heart and finish the distribution of the electrical stimuli to all parts of the ventricular walls
Although the structural components of the conduction system of the heart were known, it was Dr. Sunao Tawara (1873-1952) who discovered the AV node and described the connections between the components of what he called the "Reitzleitungssytem" (conduction system) of the heart.
The conduction system of the heart is part of a more complex rhythm control system of the heart. For more information click here.
Click on the image for a larger version. Image modified from the original: "3D Human Anatomy: Regional Edition DVD-ROM." Courtesy of Primal Pictures.
- Details
The medical term embolus arises from the Greek [έμβολο] (pronounced émvolo) meaning "a plug", or "a plunger". This Greek term was later adopted in Latin [embolus] and is used in this unchanged form today. The plural for embolus is [emboli].
In medicine, the term embolus usually refers to a free blood clot that travels down the bloodstream. When in the veins, emboli will travel easily to and through the heart. This is because veins increase in diameter towards the heart. The opposite happens in arteries. Free blood clots (emboli) that passed through the heart with no problem now enter the pulmonary arteries whose branches get smaller and smaller until the emboli plug the arterioles, and now the patient has a pulmonary embolism.
When thrombi are generated in the heart, they are usually generated in the left atrial appendage in cases of arrhythmia or atrial fibrillation. If these thrombi embolize, that is, they become free, these now emboli will continue downstream in the arteries and progressively smaller arterioles until they are bigger that the vessel and plug it, cutting off blood supply. This condition can cause an infarction, also known as a stroke.
The term embolus can also refer to liquids. fat, or gases that enter the blood stream and are not diluted.
The first use of this term in modern medicine was by Virchow in 1846 in his paper "On the Occlusion of the Pulmonary Arteries"
The root term for this word is [-embol-]. Examples of its use are:
• Embolism: The suffix [-ism] means "behavior" or "pathology".
• Thromboembolism: A combination of root terms; the root term [-thromb-] means "fixed clot" and [-embol] means "a free clot". A condition or presence of both trombi and emboli.
Sources:
1. "The Origin of Medical Terms" Skinner, HA 1970 Hafner Publishing Co.
2. "Medical Meanings - A Glossary of Word Origins" Haubrich, WD. ACP Philadelphia
- Details
- Written by: Efrain A. Miranda, Ph.D.
- Hits: 8516
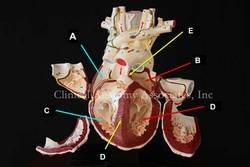 [UPDATED] The term [atrium] is Latin, its plural form is [atria]. The atrium was the center hall of a Roman home, around which the rest of the rooms opened. Since the atrium was the first area of the house that was entered once passing through the front door, the term [atrium] has been used to describe the "entrance hall', such as the atrium of a hotel. The atria are the two superior chambers of the heart. (see image, items "A=right atrium" and "B=left atrium")
[UPDATED] The term [atrium] is Latin, its plural form is [atria]. The atrium was the center hall of a Roman home, around which the rest of the rooms opened. Since the atrium was the first area of the house that was entered once passing through the front door, the term [atrium] has been used to describe the "entrance hall', such as the atrium of a hotel. The atria are the two superior chambers of the heart. (see image, items "A=right atrium" and "B=left atrium")
An interesting question is why are the atria called so, since they are part of the heart, and not just the entrance?. The reason is that early anatomists considered the heart to be composed only by the ventricles. The atria were then chambers where blood would wait before entering the "heart proper", ergo [atria].
Each atrium has a smooth wall (sinus venarum) and a muscular extension akin to a closed-end bag. These are the atrial appendages or auricles. Anatomically they are quite different. The right atrial appendage communication or opening to the right atrium is wide and allows blood to easily flow from and to the atrium. On the contrary, the left atrial appendage has a very small opening (ostium) and its morphology is convoluted with lobulations and a complicated mesh of atrial muscle wall.
The very structure of the left atrial appendage is quite conducive to the formation of clots in atrial fibrillation (AFib). These anchored clots (thrombus/thrombi) can detach and become free clots (embulus/emboli) that will enter the blood stream, pass into the left ventricle, then though the aortic valve, and then pass into the ascending aorta and main circulation. Unfortunately, two of the first arteries that arise from the aorta are the common carotid arteries that take blood to the brain and these thrombi can cause a brain stroke.
Personal note: On November 7, 2023 Dr. Randall K. Wolf invited me to a seminar where we reviewed the anatomy of the left atrial appendage, the problems it can cause in atrial fibrillation as a cause for stroke, and the reasons for its exclusion in AFib surgery.
Image property of:CAA.Inc.. Photographer:D.M. Klein
- Details
- Written by: Efrain A. Miranda, Ph.D.
[UPDATED] What is atrial fibrillation?
Atrial fibrillation (AFib) is one of the most common heart conditions, affecting 4% of the adult population. Characterized by a rapid, irregular heartbeat, AFib is largely due to abnormal electrical impulses that cause the atria of the heart to quiver when it should be beating steadily.The atria are the two upper chambers of the heart.
Because of this quivering action, blood flow is reduced and is not completely pumped out of the atria. This negatively impacts cardiac performance and also allows the blood to pool and potentially clot. These clots, if freed, can enter the systemic circulation and cause a stroke.
At rest, a normal heart rate is approximately 60 – 100 beats per minute. In a person with AFib, that heart rate can increase to 180 bpm or even higher. Thorough testing by your health care provider can spot abnormalities in the heart's rhythm before any obvious symptoms are noticed.
What are the symptoms?
Whether it is caused by stress, exercise, or too much caffeine, most people experience rapid heart from time to time. Most cases are harmless, but AFib is a serious medical condition that may often be long lasting. Some people with AFib experience no symptoms at all. But for others, AFib may cause:
- Exercise intolerance
- Fatigue
- Severe shortness of breath
- Chest pain
- Palpitations
- Light-headiness
What causes atrial fibrillation?
Your heart is divided into four chambers: the two upper chambers called atria, and two lower chambers called ventricles. In order for blood to be pumped through your body, a group of specialized cardiac cells, the conduction system of the heart, sends electrical impulses to the atria that tells your heart to contract. Contractions of the heart send approximately five quarts of blood through your body every minute. In people with AFib, however, the impulses are sent chaotically. The atria quiver instead of beat; the blood isn't completely pumped out and may pool and potentially clot. AFib is a leading cause of stroke because of the anatomy of the left ventricle. For more information, read this article.
Are you at risk?
Your chances of developing AFib increase with age. AFib occurs more commonly in women than in men. According to the Framingham Heart Study, AFib is associated with a higher risk of death for women than for men. You are also at greater risk of developing AFib if you suffer from an overactive thyroid, high blood pressure, a prior heart attack, congestive heart failure, valve disease, or congenital disorders.
Diagnosis
AFib can sometimes be diagnosed with a stethoscope during an exam by a doctor or other health care provider and is confirmed or diagnosed with an electrocardiogram (EKG). There are several types of EKG’s. They are:
- Resting EKG – Electrical activity in the heart is monitored when a person is at rest.
- Exercise EKG – Activity is monitored when a person jogs on a treadmill or exercises on a stationary bike.
- 24-hour EKG (Holter Monitor) – A person wears a small, portable monitor that detects activity over the course of a day.
- Transtelephonic event monitoring – A person wears a monitor for a period of a few days to several weeks. When AF is felt, the person telephones a monitoring station or activates the monitor's memory function. This type of EKG is particularly useful in detecting AF that occurs only once every few days or weeks. Unfortunately this type of monitor does not record heart events while you are sleeping.
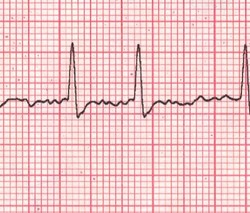
The image on this article is a typical EKG AFib recording showing the flutter of the atria followed by the ventricular contraction. In the larger image (click on the image of the article) you can see how this fluttering of the atria causes an abnormal spacing of the ventricular contractions which some patients feel in their chest.
PERSONAL NOTE: For more information on AFib and its surgical treatment, click here.
Thanks to Dr. Randall K. Wolf for the image and links