Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 1515 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

William T.G. Morton
William Thomas Green Morton (1819-1868). American dentist, was born in Charlton, MA. In 1840, He started his studies at the Baltimore College of Dental Surgery. Interestingly, he left college without graduating to study with Horace Wells, DDS, in Hartford, CT. He started Medical school at Harvard, and left without graduating. In 1852 Morton received his honorary MD degree.
In 1846, Morton was able to successfully and painlessly extract a tooth from a patient under ether administration. To this effect he used an ether inhaler of his own invention that he called “Letheon”. This led to his now-famous demonstration of the use of ether as an anesthetic on October 16,1846 at the Massachusetts General Hospital first operating room, today known as the "Ether Dome". This is the first-ever recorded use of anesthesia as a way to reduce or eliminate pain in surgery, one of the revolutions in surgery, the other being Lister’s antiseptic technique.
Morton tried, unsuccessfully, to establish a patent on his discovery against Horace Wells (1815 – 1848). The litigation costs led him to poverty and he died with no money on 1868.
Although the American Dental Association in 1864 passed a formal resolution stating that Horace Wells was the discoverer of anesthesia, the name of William TG Morton has been tied to it since.
Sources
1. “William Thomas Green Morton (1819-1868” Keys. TE. Anesth and Analg (1973) 52: (2) 166
2. ” Morton, dentist, who first publicly demonstrated ether anesthesia; a short biography” Archer WH, William TG. J Am Dent Assoc. 1946 Dec 1;33(23):1528-32
3. “Horace Wells: Discoverer of Anesthesia” Jacobsohn PH. Anesth Prog (1995) 42:73-75
4. “The last days of William Thomas Green Morton” Vandam LD J Clin Anesth (1996) Sep;8(6):431-4334
- Details
A [lung] is one of the two main respiratory organs. It is an organ filled with minute air sacs or alveoli, giving its parenchyma the look and feel of a spongy tissue. Its function is the reoxygenation of blood.
Each lung is located on each side of the thoracic cavity, each one surrounded by a serosa membrane called "pleura". The pleura forms a sac that surrounds the lung and also lines the thoracic wall. The pleura that lines the thoracic wall is called "parietal pleura", while the pleura that lines the lung is called the "visceral pleura". An extension of the visceral pleura inferior to the pulmonary hilum forms the pulmonary ligament.
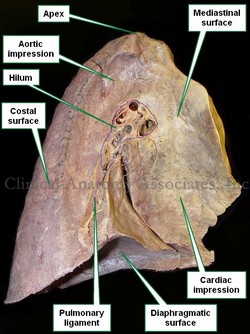
A lung has three surfaces and an apex. The inferior surface, base, or diaphragmatic surface; the medial surface or mediastinal surface, as if forms the lateral wall of the mediastinum; and the lateral or costal surface.
The lungs are also divided into lobes. The right lung has three lobes: superior, middle, and inferior while the left lung only has two lobes: superior and inferior. Because the heart has a left-sided tilt the left lung is slightly smaller than the right lung.
There are four structures that enter or leave the lung and they are found at the pulmonary hilum in the medial surface of the lung. These structures are: the main or primary bronchus, the pulmonary artery, and two pulmonary veins.
After entering the lung through the hilum each bronchus will divide into smaller and smaller bronchi eventually opening into microscopic air sacs called the alveoli. Each alveolus or alveolar sac is surrounded by capillaries. It is here where gas exchange takes place allowing for blood reoxygenation.
When examined, a lung will show the impressions of the organs that are in contact with it. Click on the accompanying image and you will be able to see the impressions left by the aorta and the heart
Image property of: Photographer: David M. Klein
- Details
The medical word [atheroma], has the root term [-ather-] arising from the Greek [ath?ra] meaning "gruel", "porridge", or "groats". This refers to the consistency of the content of a soft atheromatous plaque. The suffix [-oma] means "mass", "growth" or "tumor". A mass of soft gruel-like substance. The plural form for atheroma is [atheromata].
An atheroma is abnormal edema and accumulation of cholesterol and fatty acids with varying amount s of macrophages, fibroblasts and connective tissue in the tunica intima of an artery. It is usually covered by a “cap” of thicker, drier, yellowish fibrous material. An atheroma is a cavity filled with a fatty gruel-like material covered by a cap. Atheromatous disease is characterized by a large number of these masses in the walls of the arteries of a patient.
Atheromata are found in smaller caliber arteries can reduce the lumen of the artery leading to ischemia and in the case of the coronary arteries, myocardial infarction.
The cap in an atheroma can be dislodged by the arterial blood flow in which case the content of the atheroma is emptied into the bloodstream becoming a fatty embolus. Since arteries become arterioles and then capillaries, this fatty embolus will flow distally to the point where it will lodge, blocking blood flow.
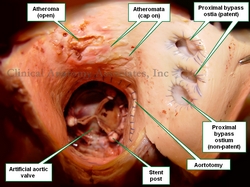
WARNING: The image of the pathology in this article is quite descriptive
The accompanying image is a clear depiction of this situation. This is a superior view of the ascending aorta. The patient in this case had an artificial aortic valve implanted and the aortotomy performed for the procedure is also indicated. The patient also had three coronary bypass grafts, one of which was clogged or non-patent. There are at least two atheromata with the cap still on. The image also shows at least one atheroma empty. This indicates that the content of the atheroma became a fatty embolus. Click on the image for a larger depiction.
Image property of: Photographer: David M. Klein
- Details
The word [calyx] is Latin, meaning "an outer covering", although it's origin is most probably Greek, from [kylix], meaning "a cup". This is the meaning we use today in medical terminology. The plural form for [calyx] is either [calyces] or [calyxes].
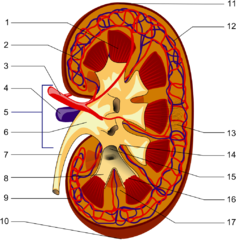
In human anatomy the term is used to denote small, cup-like extensions of the renal pelvis that help collect urine.
Each one of the minor calyces (8-20) surrounds extensions of the renal parenchyma called renal papillae. These papillae are found at the apex of the renal pyramids. This allows the urine to drip into the minor calyx as though into a cup. The minor calyces will then converge into larger calyces, each one known as a major calyx. There are between 2 to 4 major calyces in each kidney.
The major calyces then join together to form the renal pelvis, which continues with the ipsilateral ureter to the urinary bladder.
Sources
1. "Gray's Anatomy"38th British Ed. Churchill Livingstone 1995
3. "Tratado de Anatomia Humana" Testut et Latarjet 8 Ed. 1931 Salvat Editores, Spain
Images in the public domain, courtesy of Wikipedia
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

J. Marion Sims
J. Marion Sims (1813 – 1883). American surgeon and gynecologist. James Marion Sims is considered the “Father of Gynecology". He was born in Hanging Rock, South Carolina. At age 12 he moved to Lancaster, South Carolina. Sims studied at the SC College and later moved to Philadelphia, PA where he studied Medicine at the Jefferson Medical College, graduating in 1835. He returned to Lancaster to practice, but shortly after moved to Montgomery, Alabama.
In 1845 Sims started his studies to close vesicovaginal fistulas, operating in the same patient many times. He was finally able to do this using a lateral recumbent position (later called Sims’ position) and a specially designed, U-shaped, vaginal retractor (later called Sims’ speculum). For this procedure he used silver wire as suture material. His findings were published in 1852 in his paper entitled “On the Treatment of Vesico-Vaginal Fistula”
After moving to New York J. Marion Sims helped in the founding and establishing the Woman's Hospital in the State of New York in 1855. Sims moved to Europe during the American Civil War. In Europe he became well-known and in 1866 published his book “Clinical Notes on Uterine Surgery”. While in Paris Sims performed the first cholecystostomy to relieve a blocked gallbladder.
He continued his contribution to gynecology advancing uterine prolapse surgery, advocating hysterectomy for bleeding fibroids, and suggested total hysterectomy as the only means of curing uterine cancer. One of his last contributions (not well accepted initially) was the indication for immediate exploratory laparotomy in abdominal gunshot wounds, burst ectopic pregnancy and any other sharp abdominopelvic trauma.
Sims died in New York on November 13, 1883
Sims’s life was and still is the cause of controversy. His use of slave patients, his professional jealousy and egotism, and his more than once reported disdain for patient privacy would not be accepted by today’s standards. Today in Lancaster his name helps the community thorough the “J. Marion Sims Foundation” dedicated to “support prevention and educational programs that help the citizens of Lancaster and the communities of Great Falls and Fort Lawn”
Sources:
1. “The Influence of J. Marion Sims on Gynecology” Heaton CE Bull N Y Acad Med 1956 32 (9): 685–688
2. “J. Marion Sims, the Father of Gynecology: Hero or Villain?” Sartin, JS South Med J 2004;97(5):500-505
3. “J. Marion Sims: A Defense of the Father of Gynecology” O’Leary JP South Med J 2004;97(5):427-429
4. “Carl Langenbuch and the First Cholecystectomy” Traverso LW Am J Surg 1976; 132; 81-82
- Details
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
The Latin word [caput] means "head" and the word [medusae] is also Latin and means "Medusa's". [Caput medusae] means "Medusa's head". Medusa is a Greek mythological figure, ruler of the Gorgons; in her mortal form she had a head covered with snakes and looking into her eyes would cause an observer to turn into a stone statue. She was killed by Perseus who used a shield to see her reflection without turning to stone and was thus able to cut her head off.
The term [caput medusae] is used in medical terminology to denote a medical sign, a crown of engorged veins that radiate from the umbilicus. These engorged veins are caused by increased hepatic portal pressure (portal hypoertension) which causes retrograde flow in the veins from the abdominal cavity to the superficial cutaneous veins, engorging them.
The caput medusae sign is usually seen in patients with advanced hepatic cirrhosis.
WARNING: The following explicit images show different stages of this sign. Each of the following links will open images in separate screens and web sites: Image 1; Image 2; Image 3; Image 4.
Medusa's head image in the public domain courtesy of Wikipedia. All other images are the property of each website. We only provide the links to them.