Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 964 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.
Giulio Cesare Aranzio (1530 -1589) Italian surgeon and anatomist. Born in Bologna, Giulio Cesare Aranzio is better known by the Latinized version of his name Julius Caesar Arantius. His Italian last name is sometimes spelled Aranzi.
Born in a poor family, Aranzio began his medical studies under the tutelage of his uncle, Bartolommeo Maggi (1477 – 1552), studied medicine at the University of Bologna where he graduated MD in 1556. The same year he became a Professor of Anatomy and Surgery at the in 1556. Arantius was the first lecturer at the University of Bologna to hold a separate professorship of anatomy. Before him, the University would allow any surgeon to perform dissection and lectures.
Arantius had several publications that include:
• Observationes Anatomicas (Anatomical Observations)
• De Humano Foetu Opusculum (On the Human Fetus)
• De Tumoribus Secundum Locos Affectos (Tumors according to the affected places)
• Hippocratis librum de vulneribus capitis commentarius brevis (Short commentary on Hippocrates’ book on head wounds)
Arantius was the first to describe the foramen ovale (fossa ovalis) and the ductus arteriosus, discoveries that were later erroneously ascribed to Leonardo Bottalus (Botal). He also described the nodules in the leaflets of the aortic valve that today bear his name (nodules of Arantius) which he described as being “cartilaginous” in nature. This is not as farfetched as it seems as these nodules can become hypertrophic and harden with age. Arantius was also the first to describe the hippocampus, a formation on the brain associated with the limbic system, mood disorders, and depression.
Arantius was a consummate anatomist and a great surgeon. Apparently he treated nasal polyps, performed nasal reconstructions and a number of surgeries ahead of his time. One of his great anatomical observations was that the blood in the heart did not pass through “invisible pores” in the interventricular septum, but rather exits the heart through the pulmonary trunk, setting the stage for the discovery of circulation by William Harvey (1578 – 1609)
We have not been able to find a portrait of Arantius and the only reference is a a bust with the name “Aranzio” located at the Biblioteca comunale dell'Archiginnasio in Bologna, Italy. The bust is found in the anatomical amphitheater, built in 1637. Unfortunately, the theater was severly damaged in January 29, 1944 during WWII. It has been meticulously restored over the years. Here is an article (in Italian) on the amphitheater.
Sources:
1. “Giulio Cesare Arantius (1530-1589): a surgeon and anatomist: his role in nasal reconstruction and influence on Gaspare Tagliacozzi” . Gurunluoglu R, Gurunluoglu A Ann Plast Surg. 2008 Jun;60(6):717-22
2. “Giulio Cesare Aranzio (Arantius) (1530-89) in the pageant of anatomy and surgery” Gurunluoglu R, Shafighi M, Gurunluoglu A, Cavdar S. J Med Biogr. 2011 May;19(2):63-9
3. “Hippocampus – Why is it studied so frequently?” Radonjic, V. et al Vojnosanit Pregl 2014; 71(2): 195–201
4: “The history of Bologna University's Medical School over the centuries, A Short Review” Moroni, P. Acta Dermatoven APA Vol 9, 2000, No 2 73-75
- Details
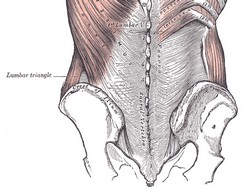
The [lumbar triangle] is a well-defined triangular space in the posterolateral lumbar region. Also known as the inferior lumbar triangle, its boundaries are: inferior, the iliac crest; anteromedial: latissimus dorsi muscle; posterolateral: posterior border of the external oblique muscle. The triangle has a superior apex, and the floor of the triangle is the internal oblique muscle.
The triangle is named after Jean-Louis Petit (1674 - 1750), a French Surgeon who is said to have been an anatomy teacher at an early age and became a surgeon when he was only eighteen!
The lumbar triangle is an area that is not as thick as the rest of the abdominal wall and as such it is a site of potential weakness that can lead to a lumbar hernia, also known as Petit’s hernia.
Sources:
1. “Jean Louis Petit – A Sketch of his Life, Character, and Writings” Hayne, AP San Fran Western Lancet 1875 4: 446-454
2. “Oeuvres compl?tes de Jean-Louis Petit” 1837 Imprimerie de F. Chapoulaud
3. Extraits de l'eloge de Jean-Louis Petit Ius dans Ia seance publique de I' Academie Royale de Chirurgie du 26 mai 1750” Louis A. Chirurgie 2001: 126 : 475- 81
- Details
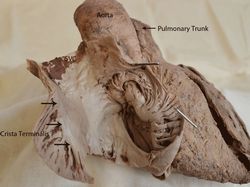
The anatomical term [crista terminalis] is Latin. [Crista] refers to the crest of a helmet, a tuft (of hair or feathers), or a ridge. The word [terminalis] means "end" or "terminal". The term then means "the terminal or end ridge".
The crista terminalis is a superoinferior muscular ridge found in the right atrium marking the boundary between the smooth wall of the right atrium, also known as the "sinus venarum" (venous sinus), and the muscular wall of the right atrial appendage. The muscular wall of the right atrial appendage is comb-shaped and is called the pectinate muscle.
Because of the longitudinal direction of the muscular fibers of the crista terminalis, it is considered to be one of the internodal pathways for electrical transmission of the cardiac depolarization between the sinoatrial (SA) node and the atrioventricular (AV) node.
The crista terminalis causes a superoinferior longitudinal depression on the surface of the heart known as the sulcus terminalis.
The accompanying image is a dissection of a human heart and shows the crista terminalis, pectinate muscle, fossa ovalis, the ostium of the coronary sinus, the right atrial smooth wall of the sinus venarum. Click on the image for a larger version. The animated image does a slow pass trough all these and other structures.
Sources:
1. "The origin of Medical Terms" Skinner, AH, 1970
2. "Terminologia Anatomica: International Anatomical Terminology (FCAT)" Thieme, 1998
3. "Tratado de Anatomia Humana" Testut et Latarjet 8th Ed. 1931 Salvat Editores, Spain
Image courtesy of Rocky Vista University,College of Osteopathic Medicine, Parker, CO
- Details
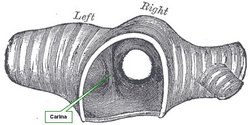
The word [carina] is Greek, from [καρίνα] meaning “keel”, as in the keel of a boat.
The carina is an anteroposterior elevation found at the point of bifurcation of the trachea into the left and right bronchi. When looking at it from the superior aspect, it does look as if you were looking at the keel of boat from the bottom up, and this is the image that endoscopists see when looking at this area. See the accompanying image.
The bifurcation of the trachea and the carina are usually found at the level of the sternal angle (of Louis), which is about the level of the superior border of the 5th thoracic vertebra.
Since the right bronchus is slightly wider than the left bronchus, the carina is usually slightly displaced to the left of the midline.
The lymph nodes that surround the area of the bifurcation of the trachea, and inferior to the bifurcation are called the carinal nodes.
- Details
Although not a medical term per se, we use the word [vernacular] constantly on this blog to refer to terms used commonly or colloquially by non-health care professionals.
Merriam-Webster’s definitions of [vernacular] are multiple, all pointing to common usage by a group:
• of, relating to, or using the language of ordinary speech rather than formal writing
• of, or relating to the common style of a particular time, place, or group
• using a language or dialect native to a region or country rather than a literary, cultured, or foreign language
• of, relating to, or being a nonstandard language or dialect of a place, region, or country
• of, relating to, or being the normal spoken form of a language
• applied to a plant or animal in the common native speech as distinguished from the Latin nomenclature of scientific classification
This last definition is the one that applies mostly to what we mean in this blog. While we may use the anatomical term “rectus abdominis” , most people would say “six-pack” – which is wrong on two aspects: it is vernacular, and it is not a “six pack”, if you count them, you will see that a well-developed rectus abdominis has eight bellies, four on each side, making it really an “eight pack”!
Another one would be the vernacular term "pinky" to refer to the fifth digit of the hand. Yet another one would be the use of the vernacular term “stomach” to refer to the abdomen, that is one of my pet peeves!
- Details
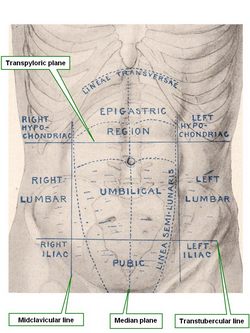
UPDATED: The word [hypochondriac] is formed by the prefix [hypo-], meaning "below", the root term [-chondr-], meaning "cartilage", and the adjectival suffix [-iac], meaning "pertaining to". A literal translation would be "pertaining to (the area) below the cartilage"; this does nothing to explain what we understand as a "hypochondriac" patient.
The word [hypochondrium], was first used by Hippocrates of Cos (460 BC - 370 BC) to denote the anterior bilateral areas below the lower costal cartilages of the thorax, what we known today as two of the abdominal regions, the hypochondriac regions.
These two areas contain on the right, the liver and gallbladder, and on the left, the spleen, part of the stomach, and the left flexure of the colon. Because of the visceral sensations referred by some patients in these areas without any apparent problems, these symptoms started to be called "hypochondriac symptoms". It did not take much time to refer to a patient that refers pathological symptoms without being sick as an "hypochondriac". The first one to actually use this term in a publication was Robert Whytt (1714 - 1766), a Scottish physician.